When you are trying to start a family, miscarriage is one of the most heartbreaking things that can happen.
It’s happened to me. In the nearly 6 years that we’ve been growing our family, I’ve suffered from recurrent miscarriage–3 miscarriages, 2 beautiful babies, and then 3 more miscarriages.
Most of mine have been what are called “chemical pregnancies”–that is, they’re so early that the only way you can tell I’m pregnant is by the hCG in my bloodstream. (That’s also why I’ve decided not to test early for pregnancy anymore.)
It’s devastating. From the moment you first see those two pink lines on the pregnancy test, you start to hope and dream. You think about what it will be like to hold and talk to your baby.
You imagine their future.
When you miscarry, you don’t just lose a pregnancy. You lose an entire future.
So I know you’re wondering, “What causes miscarriage? And is there anything I can do to prevent recurring miscarriage?”
What Causes Miscarriage?
The question I’ve found myself repeating over and over again after my miscarriages is “Why? Why, God, did this child not make it?”
The first thing I want you to tell yourself is that it’s not your fault. I know it’s easy to blame yourself, to wonder what you should have done differently.
But please don’t do that. Processing your grief is hard enough without blaming yourself for something that isn’t your fault.
Doctors don’t always know what causes a miscarriage, but there are many possible causes. And most of the time there’s nothing you could have done to stop it.
Here are the most common causes of miscarriage.
1. Chromosomal defects
Sometimes when a sperm and egg join up, there are problems with the chromosomes.
Every time a new human is conceived, genetic defects are passed on to the baby from both its father and its mother. Many of those defects have little-to-no effect. Others result in conditions such as Downs syndrome. And others prevent survival altogether.
Researchers agree that in the majority of cases, miscarriage is due to one of these defects.
Because our bodies tend to accumulate these defects as we age, this kind of miscarriage happens even more frequently in older couples as the woman’s egg health deteriorates. The man’s sperm may also be less healthy as he gets older.
If you find yourself in the “older couple” bracket, Hethir at Natural Fertility Info says it’s possible to improve your egg health naturally. A few of her suggestions are similar to what I suggest in my article on balancing your hormones naturally, plus she offers a few other helpful tips as well.
2. Uterine abnormalities
I have a mildly bicornuate uterus, meaning my uterus is shaped like a heart.
Thankfully it hasn’t affected my two full-term pregnancies, but it is the sort of thing that can affect progesterone production or, in more extreme cases, implantation and baby growth.
Uterine abnormalities like this are referred to as “anatomical causes.”
Anatomical causes include
- misshapen uterus: an abnormally shaped uterus can restrict a baby’s growth or prevent proper implantation
- incompetent cervix: the opening of the cervix is weak and opens earlier than it should
- uterine fibroids: large fibroids can change the shape of the uterus, making implantation difficult; they can also divert bloodflow away from the developing baby
- Asherman syndrome: most common in women who have had several D&C operations, this syndrome refers to the accumulation of scar tissue in the uterus
3. Hormone imbalance
There are several hormone imbalances that can contribute to recurrent miscarriage.
Low progesterone
The most important hormone for maintaining a healthy pregnancy is progesterone. When you have low progesterone, your body cannot form a sufficient uterine lining and cannot support a pregnancy.
Often you can tell if your progesterone is low by charting your cycles with natural family planning. You will see a short luteal phase (from ovulation to your next period), also known as a “luteal phase defect.”
High estrogen can also contribute to low progesterone.
High or low thyroid
Another common hormone imbalance that can cause miscarriage is hypothyroidism (thyroid is too low) and hyperthyroidism (thyroid is too high). Low progesterone and low thyroid are often linked, so if you know you have one, it’s worth looking into the other.
After my sixth miscarriage, I learned that my body was producing antibodies in line with autoimmune-induced hypothyroidism, also called Hashimoto’s thyroiditis.
All of your body’s hormones are in a delicate balance, so when one is off balance, it can throw off the others. In the case of thyroid, if it’s too high or too low, it can interfere with the production and functioning of your reproductive hormones.
High prolactin
Prolactin is the hormone that causes your body to produce milk for your new baby–it’s great if you have a baby to feed, but if you’re trying to get pregnant, too much prolactin can keep you from getting pregnant or staying pregnant.
Prolactin suppresses your body’s ability to produce estrogen and progesterone.
Insulin imbalance
A third hormone that can contribute to miscarriage when it’s imbalanced is insulin. If your body is resistant to insulin, you may develop diabetes. Uncontrolled, diabetes can lead to miscarriage.
Insulin imbalance also raises blood sugar, estrogen, and testosterone while suppressing progesterone and is a common risk factor in PCOS.
4. Blood clotting disorders
After my second miscarriage, my OB ordered a panel of tests. One of the results that came back is that I am one of the estimated 4 to 7 percent of people with a genetic defect called Factor V Leiden.
This particular defect puts me at a greater risk for blood clotting. Researchers believe that this and other clotting disorders may cause tiny clots in the uterus, which prevent blood from reaching the developing baby.
High homocysteine levels can have a similar effect. Homocysteine is an amino acid that, in high concentrations, can cause blood clotting. An Italian study in 2007 showed a correlation between recurrent miscarriage and high homocysteine levels.
Your doctor can order a blood test to determine if your homocysteine levels are too high or if you have any other clotting disorders.
5. Immune system disorders
Sometimes the mother’s immune system thinks the growing baby is a threat and attacks in self defense. At least one study shows that a particular form of enzyme therapy may help prevent this form of miscarriage.
There are also autoimmune diseases, such as lupus and Sjogren’s syndrome, that can contribute to recurrent miscarriage. These diseases makes you more prone to antiphospholipid antibodies, which cause blood clots.
6. Lifestyle habits
Drug use, excessive alcohol, excessive caffeine, marijuana, and tobacco can all contribute to miscarriage, as can pollution from living in a city.
7. Infection
Certain infections may cause miscarriage. These include
- bacterial vaginosis
- chlamydia
- gonorrhea
- HIV
- herpes (HSV)
- syphilis
- e. coli
- listeria
- salmonella
- toxoplasmosis
- rubella
What is your risk of miscarriage?
After the 12th week of pregnancy, many women breathe a sigh of relief. That’s because your risk of miscarriage drops significantly after the first trimester. (This is also why many women choose not to announce their pregnancy early.)
Expecting Science gives a fantastic scientific analysis of the available data on miscarriage risk, but here’s a quick summary.
According to a study of 668 pregnancies, the following is your risk of miscarriage between weeks 6 and 9:
- 6 weeks: 10.3%
- 7 weeks: 7.9%
- 8 weeks: 7.4%
- 9 weeks: 3.1%
If you are 35 or older, this study of 384 pregnancies shows that your risk of miscarrying by the end of the first trimester is closer to the following percentages:
- 35-37: 2.8%
- 37-39: 7.5%
- 40+: 10.8%
If you’ve miscarried in the past, your risk of recurrent miscarriage is slightly higher, but it’s not as troubling as some statistics will have you believe.
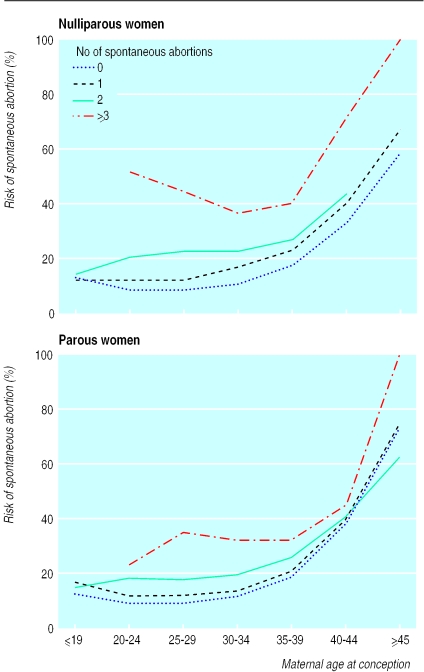
This chart from a study of over a million pregnancies shows that even if you’ve miscarried before, your chances of carrying a pregnancy to term are still generally better than 80%, especially if you’ve had fewer than 3 miscarriages.
(A note on this chart: “nulliparous” means you’ve never given birth before, and “parous” means you’ve carried at least one pregnancy to term.)
Reducing Your Risk of Miscarriage
Before we get into this part, I want to say this again: it’s not your fault. Even if you do everything right, sometimes there are factors beyond your control.
But I do want to give you some tips that can help you reduce your risk. I want to help you get into that 80% of pregnancies that go full term after miscarriage.
1. Make lifestyle changes
The first and most obvious changes you can make to reduce your risk of recurrent miscarriage is to quit smoking, quit any drugs, and stop drinking alcohol.
If you drink large amounts of coffee, tea, and/or soda, cut back on the caffeine. Studies show a definite link between excessive coffee consumption and miscarriage.
Some studies show that up to 150 mg of caffeine has very little effect on your miscarriage risk. The Bump has some great charts for helping you figure out exactly how much coffee or tea that is, but in general it’s around a cup or two of coffee per day.
If, however, you want to be absolutely sure that you’re eliminating anything and everything that could possibly cause a miscarriage, you might consider cutting out coffee completely. This meta-analysis indicated that even 2 cups of coffee a day could increase your risk of miscarriage by 8%.
I know. I love coffee too, and I hate to read that.
But, like giving up that glass of wine while you’re pregnant, giving up the caffeine at least while you’re trying to conceive and through your first trimester may be worth it.
2. Take your B vitamins
Increased homocysteine levels and low progesterone levels may be connected with low levels of vitamin B12 and B6, respectively. This Egyptian study concluded that supplementing with B12 may improve your odds of a full-term pregnancy.
B9 (folate) can reduce your baby’s risk of developing midline (neural) defects. Just make sure it’s food-derived folate and not synthetic folic acid.
Many foods, such as leafy greens, are excellent sources of folate. You can also buy a vitamin that contains real folate.
Many people’s bodies, especially those with the MTHFR gene mutation, cannot do the enzyme transformation necessary to use synthetic folic acid. But the synthetic folic acid still fills their folate receptors so that their bodies don’t get the real folate they need. (Read this study for more on the problem.)
You’ll also want to stay away from “enriched” products (such as flour and cereals) since they are usually enriched with synthetic folic acid.
As a bonus, B vitamins are just all-around good for your body. B12 can boost your energy levels, and B6 can help reduce morning sickness.
I personally take Young Living’s vitamin B complex daily.
3. Balance your hormones
Many times miscarriage is the result of hormone imbalance. If you suspect this is the case for you, take a look at my post on how to balance your hormones naturally.
I’ve seen a lot of success with normalizing my cycles using the keys in that post, and I believe it’s the reason my pregnancy with my daughter went so smoothly. I “fell off the wagon” a bit after she was born, and I believe that was a major contributor to my most recent miscarriages.
Those last two miscarriages were a big wake up call that I really needed to get back on track keeping my hormones balanced.
4. Watch your diet
Your diet is foundational to your health. “You are what you eat” isn’t just a saying–it’s the truth.
The building blocks your body needs to survive and thrive are found iny our food.
A diet high in fresh fruits and vegetables, water, and clean animal products (no hormones or antibiotics) goes a long way toward healing your body and balancing your hormones. When your hormones are balanced, you reduce your risk of recurrent miscarriage.
This article from Natural Fertility Info provides an excellent starting point for eating a “fertility diet.”
If you want to get even more in depth on diet and how it affects your fertility, I also recommend you check out Alissa Vitti’s WomanCode. She gives a clear, step-by-step guide for what to eat during each phase of your female cycle.
Or, for a more simplified approach to eating that my family has adopted, check out my template for a healthy diet.
5. Maintain a healthy weight
When you’re eating a healthy diet, a healthy weight often follows.
As a guideline, you’ll want to be sure your BMI isn’t too high or too low–a BMI over 30 or under 18 increases your risk of miscarriage. Being too heavy means your body may produce too much estrogen; having too little body fat can prevent your body from producing enough estrogen.
If you’re having trouble losing or gaining weight, you might want to talk to a dietician to come up with a diet and exercise plan.
6. Watch out for infection
Since certain infections can cause miscarriage, it makes sense to watch out for situations that could expose you to those infections.
Avoid food-borne infections by washing and cooking your food thoroughly. Avoid sexually transmitted diseases by being smart about your sexual decisions. Cleaning the cat litter box can expose you to toxoplasmosis, so have someone else do that chore while you’re pregnant.
7. Reduce stress
When you’re stressed, your body takes the pregnenolone (a precursor hormone) that it would normally use to produce progesterone and uses it to make cortisol instead.
Your body needs progesterone to maintain a healthy pregnancy, so you need to reduce that stress as soon as possible, as much as possible.
If you’re in a stressful work situation, maybe it’s time to talk to your boss about a change. If you’re experiencing stress at home, have a good talk with your partner about ways you can reduce that stress.
Try to get enough sleep and manage your time wisely.
8. Ask your doctor about miscarriage testing
Since some miscarriages are the result of genetic or physical abnormalities, it can be helpful to get tested for possible causes of miscarriage.
Knowing any potential causes will also help you know which areas to target to reduce your risk of miscarriage in the future.
Some tests you may ask for include
- Hysterosalpingogram (HSG): a dye-contrast X-ray of the uterus. This test will help you and your doctor know if your tubes are blocked, or if there are any growths or abnormalities in the shape of your uterus.
- Hormone levels: you’ll want to know if your hormone levels are normal since certain imbalances can cause miscarriage. You should know the following hormone levels:
- estrogen
- progesterone
- thyroid
- Clotting disorders: your doctor may test you for Factor V Leiden, homocysteine levels, and antiphospholipid syndrome (APS), all of which can cause blood clots. Your prothrombin time will also show how fast your blog clots.
- Other genetic disorders: some doctors may test for other genetic abnormalities, including the MTHFR mutation, which affects your body’s ability to use folic acid.
9. Try fertility-supporting supplements
In addition to a supplement containing B6, B9 (folate), and B12, you may try some natural supplements that have been shown to promote fertility and may help prevent recurrent miscarriage. My two favorites are vitex and maca.
Vitex
Vitex, also known as chasteberry, may help boost progesterone levels.
There is some debate over its safety during pregnancy, but The Essential Guide to Herbal Safety (Mills & Bone, 2005) says it can be used cautiously “in the early stages, for corpus luteal [progesterone] insufficiency.”
Maca
Maca is a root-like vegetable found in Peru, where it has been used for centuries to promote general health. It can promote fertility in both men and women.
In women, maca balances progesterone and estrogen levels.
If you take maca, be sure it’s organic from Peru and gelatinized (starch removed) for easier digestion.
Conclusion
Sometimes there’s nothing you can do to prevent a miscarriage. Most of the time there are chromosomal abnormalities at play or other factors that you have no control over. But there are a few things you can do to help reduce your risk of recurrent miscarriage.
- Make necessary lifestyle changes.
- Take B vitamins.
- Balance your hormones.
- Eat a fertility-friendly diet.
- Maintain a healthy weight.
- Watch out for infection.
- Reduce stress.
- Get miscarriage testing.
- Use natural supplements.
I know firsthand how painful miscarriage is, so I sincerely hope this article was helpful for you and that you go on to have a full-term healthy pregnancy.

Baby dust!
Was this useful? Please pin to Pinterest!
14 thoughts on “On Being a Childless Mother: Understanding and Preventing Recurrent Miscarriage”